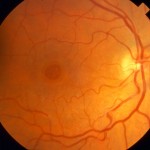
Macular Pucker
Causes of a Macular Pucker
Macular puckers often develop on their own as a part of the natural aging process. Particles that have drifted into the vitreous (the gel that fills the eye) settle onto the macula and begin to obscure vision. Membranes may also result from eye conditions or diseases such as diabetic retinopathy, retinal detachment, inflammation, injury or vascular conditions. These are called secondary epiretinal membranes, whereas spontaneously formed membranes are called idiopathic.
Symptoms of a Macular Pucker
Many macular puckers do not disrupt vision. Thicker puckers can create wrinkles or puckers in the macula resulting in some of the following symptoms:
- Blurry or distorted vision
- Straight lines appear as wavy lines
- Difficulty with fine detail or print
A macular pucker typically affects one eye. Vision loss varies based on the thickness of the pucker. Peripheral vision is not affected and there is no risk of blindness.
Diagnosis of a Macular Pucker
After a thorough examination of the eye, the physician will perform a series of diagnostic tests. These tests may include:
- Dilated eye examination
- Fluorescein angiography
- Optical coherence tomography (OCT)
Treatment of a Macular Pucker
While some macular puckers heal on their own, surgery is recommended for those that do not. Vitrectomy is performed as an outpatient procedure with local anesthesia. During the procedure, the vitreous gel is removed and replaced with a saline solution that will fill the eye and lift the pucker away from the macula. There is no non-surgical alternative to treat a macular pucker.
Macular Hole
Causes of a Macular Hole
A macular hole often develops as part of the natural aging process, when the vitreous gel thins and separates from the macula. This can pull on the macula causing a hole to form. Macular holes can also develop from:
- Injury
- Inflammation
- Nearsightedness
- Retinal detachment
- Other eye diseases
Symptoms of a Macular Hole
In its early stages, a macular hole may cause a small blurry or distorted area in the center of vision. As the hole grows over time, central vision progressively worsens. Peripheral vision is not affected. There are three different stages of a macular hole, including foveal detachments, partial-thickness macular holes and full-thickness macular holes. Each stage can progress to the next if left untreated.
Treatment of a Macular Hole
While some macular holes resolve on their own, in most cases surgery is required to effectively restore vision. Most macular holes can be successfully treated through a vitrectomy, a procedure to replace the vitreous gel with the injection of a gas bubble to help close the hole. Vitrectomy is performed on an outpatient basis under local anesthesia and is considered a safe and effective treatment for a macular hole.
Retinal Vascular Diseases
Retinal vascular diseases involve some type of problem with the blood vessels of the retina. While there are a number of different conditions that fall into this category, one of the most common forms of retinal vascular disease is retinal vein occlusion.
The retina is a thin sheet of nerve tissue located in the back of the eye where light rays are focused and transmitted to the brain. Tiny blood vessels supply the retina with oxygen and other nutrients. Arteries deliver blood and the retinal veins carry it. Sometimes one of these arteries hardens or swells and presses on a nearby vein. The vein can then become blocked, or occluded, making it difficult for blood to leave the eye. This condition is called a retinal vein occlusion, or RVO. A retinal vein occlusion is also known as venous stasis retinopathy or hemorrhagic retinopathy. The blocked circulation caused by a retinal vein occlusion can lead to:
- Swelling
- Bleeding
- Growth of abnormal blood vessels
- Partial or total vision loss
Retinal vein occlusions are the second most common cause of blood vessel-related vision loss, the first being diabetic retinopathy. A retinal vein occlusion typically occurs in men and women over the age of 50, particularly those in their 60s and 70s.
Retina - Vitreous Disease
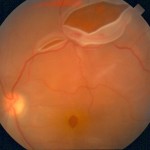
Conditions of the the retina and vitreous can lead to loss of vision and blindness. Some of these conditions include the following:
- Retinal tear
- Retinal detachment
- Macular degeneration
- Diabetic retinopathy
- Infection
- Trauma
Early detection and treatment is essential before vision is lost and to prevent further deterioration.
Hereditary Eye Diseases
Conditions that affect the eye usually can be attributed to either an infection, injury or a complication of another illness or disease. While not very common, there are several eye diseases to which patients are genetically predisposed. These diseases can affect the eye muscles, tear drainage system, cornea, lens and retina. They may cause difficulty focusing, vision loss or even blindness. Some of these conditions are present at birth, while others do not develop until much later in life.
In order to diagnose any potential conditions as early as possible, regular eye exams are recommended for those patients whose parents have been affected by a hereditary eye disease.
Hereditary ophthalmic diseases in children may include some of the following:
- Congenital cataracts
- Congenital glaucoma
- Retinal degeneration
- Optic atrophy
- Eye malformations
- Strabismus
Hereditary ophthalmic diseases in adults may include the following:
- Retinitis pigmentosa
- Glaucoma
- Age-related macular degeneration
With regular ophthalmic examinations, early diagnosis and treatment can address the complications of the disease so that it can be managed effectively.